The Risk of Becoming Allergic to Meat After a Tick Bite May Be Higher Than Thought

The tick menace is even worse than we thought. A pair of new studies this month suggests that there are more tick species out there in the U.S. that can cause an unusual form of allergy to red meat.
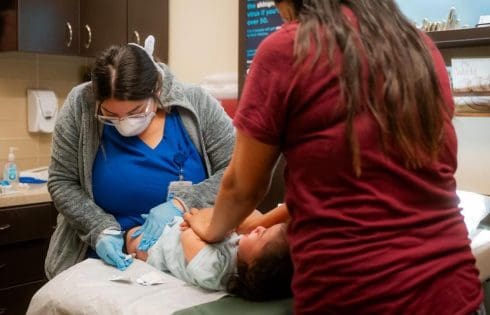
Scientists from the Centers for Disease Control and Prevention and local health officials published the research late last week in the journal Emerging Infectious Diseases. The studies detail cases of red meat allergy, formally known as alpha-gal syndrome, tied to bites from two tick species not normally associated with it—ticks that also cause Lyme disease. These cases seem rare, but indicate that more people are at risk for the syndrome than currently assumed.
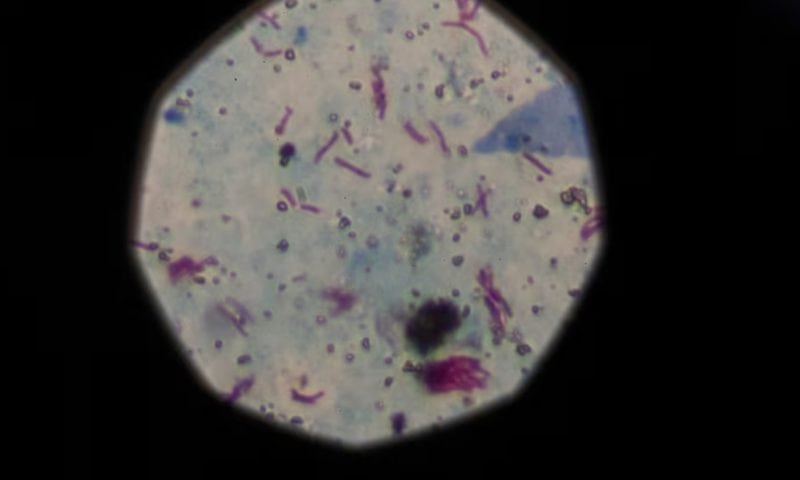
Alpha-gal is a sugar found in the muscles of most mammals, though importantly not humans. We can normally tolerate the alpha-gal found in the meat we eat without issue. But for reasons we’re still trying to understand, a tick bite can sometimes cause our bodies to develop an overactive immune response to alpha-gal, essentially making us allergic to red meat and even dairy. Alpha-gal syndrome is the only type of classic food allergy that involves a sugar (the alpha-gal) rather than a protein. And unlike other food allergies, symptoms might take hours, not minutes, to show up after exposure.
In the U.S., alpha-gal cases are nearly always associated with the bite of a lone star tick (Amblyomma americanum), which is predominantly found throughout the eastern half of the country. But there are different tick species known to cause it in other parts of the world, and doctors stateside have encountered the occasional case in places where the lone star shouldn’t be residing.
In this latest research, scientists have discovered at least two, but possibly more, cases of alpha-gal that don’t fit the typical description.
In one study, researchers documented a woman in Washington who developed alpha-gal in 2017, following a bite from an unknown species of tick. As a result, she switched to a vegetarian diet. Three years later, she got a second tick bite. Though she avoided any symptoms because of her diet, blood tests showed a dramatic rise in antibodies to alpha-gal. This time, she was able to collect the tick for testing, identified as Ixodes pacificus, or the western black-legged tick. Two years later, she got another bite from an I. pacificus tick and once again experienced a rise in alpha-gal antibodies. Importantly, the woman also reported no recent travel history to places where the lone star tick is found.
In the second study, researchers traced back a case of alpha-gal in Maine likely caused by the bite of an Ixodes scapularis tick, or deer tick. Though lone star ticks have rarely been found in Maine, they’re not thought to have established a local population in the area, according to the researchers. Despite this, they were able to find 23 confirmed cases of red meat allergy reported to the state dating back to 2014. While some people could have caught these cases while traveling in areas endemic to the lone star tick, several people reported no such travel.
The “findings might reflect a limited role for tick species other than A. americanum in [alpha-gal syndrome] development in the United States, which is further supported through review of geographic distribution of suspected cases and range of A. amblyomma ticks,” the authors wrote in one paper.
That said, most cases of red meat allergy in the U.S. are still reported in places where the lone star tick is found. Lab experiments have also supported the idea that these ticks are more likely to cause the allergy than other species in the U.S. But both Ixodes ticks are widely distributed through regions of the U.S. and are already known to spread nasty diseases like Lyme to people.
Though alpha-gal cases caused by Ixodes ticks might be rarer than the classic version, the overall incidence of the syndrome is climbing. A study in 2023 from the CDC and others estimated that up to 450,000 Americans have developed alpha-gal syndrome since 2010, with rates likely increasing over that time period as well. So if more ticks besides the lone star can cause the condition, then people and doctors in parts of the country where it isn’t commonly found should at least be aware of the possibility, the researchers say.