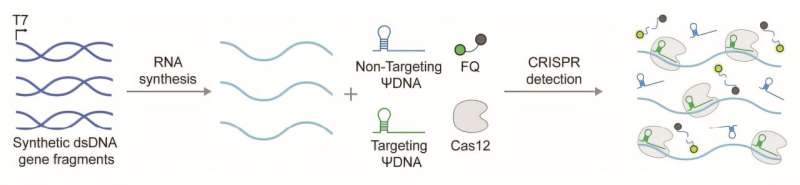
A team of engineers at the University of Florida has developed a new form of CRISPR technology that could make diagnostics and treatments safer, more precise, and more affordable, while opening the door to entirely new ways of controlling disease.
Published in Nature Biotechnology, the work establishes the world’s first system that uses DNA, rather than RNA, to guide CRISPR enzymes to its target, overturning the long-standing paradigm.
To understand why that matters, it helps to think of how cells work.
Inside every cell is DNA, the body’s master instruction manual. But cells don’t use that original blueprint directly. Instead, they make working copies, or RNA, that carry instructions to build proteins and carry out functions.
“Those RNA copies are like Xerox copies of the original manual, and sometimes those copies have errors,” said Piyush Jain, an associate professor and the Shah Rising Professor in the department of chemical engineering at UF and the study’s lead author.
Those errors can have serious consequences. In diseases such as cancer, cells can produce too many faulty copies or follow incorrect instructions, leading to uncontrolled growth or other problems.
How current CRISPR tools fall short
For years, scientists have used CRISPR to target and cut genetic material, often focusing on making permanent changes to DNA itself. More recently, researchers have developed tools to target RNA, what Jain called the working copies, offering a way to intervene without altering the underlying genetic code.
But those approaches come with tradeoffs, he said.
“Existing RNA-targeting CRISPR systems rely on RNA guides to find their targets,” Jain said. “While effective, they can sometimes affect unintended molecules, creating off-target effects. They can also be costly and less stable.”
The shift to DNA-guided targeting
The new system takes a different approach.
Instead of using RNA as a guide, the team engineered CRISPR to use DNA, which is naturally more stable and easier to produce. This allows the system to more precisely identify and act on specific RNA molecules inside the cell.
In practical terms, that means scientists can focus on correcting or controlling the “Xerox copies” without disturbing the original blueprint.
“It gives us a way to fix or tune the instructions the cell is using in real time, without immediately changing the DNA,” Jain said.
That added level of control could be important for patient safety. By targeting RNA first, scientists may be able to reduce harmful activity, like disease-causing signals, before deciding whether permanent genetic edits are necessary.
The team also found that their system drastically reduces unintended effects compared with existing approaches, improving precision by orders of magnitude in some cases.
Lower costs and wider impact
Beyond precision, the new technology could also lower costs.
“DNA guides are far cheaper and easier to manufacture than RNA guides, and they are far more stable,” Jain said. “While RNA molecules degrade quickly, DNA can remain intact for long periods.”
Together, those advantages could make CRISPR-based tools more accessible for both research and clinical use. The breakthrough tool simplifies clinical diagnostics by catching viruses like HIV early and detecting hepatitis C with 100% accuracy.